Atrial Fibrillation

What is atrial fibrillation?
What causes atrial fibrillation?
How common is AFib?
How come some people with AFib don't even know it?
What tests are done?
How is AFib treated?
What if those things don't work?
What about cardioversion? That sounds scary!
What are some of the medications used to treat AFib?
What sorts of blood thinners are you talking about?
How long do I have to take a blood thinner?
Why can't I just take an aspirin?
Why won't they just put in a pacemaker. That will fix it, won't it?
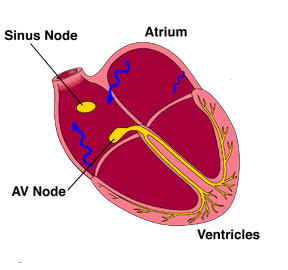
While atrial fibrillation causes inefficiency of the heart, it is well tolerated by many patients. Importantly, it has become increasingly clear that it can be associated with an increased risk of stroke. Therefore, control of the arrhythmia or the administration of blood thinners has become an important goal, and one that is best not ignored. Treatment is not "cookbook" and care and judgment must be used to choose the right therapy, a situation that can often be frustrating to the people who have the arrhythmia.In the sections on arrhythmias, we described the normal sequence of electrical activity of the heart as a regular process, spreading out as a predictable wave of stimulation throughout the heart, leading to coordinated muscle contraction. In atrial fibrillation, that regular wave does not occur in the upper chambers of the heart. There is no single pacemaker starting the process. Instead, the electrical activity moves about randomly, depolarizing the next tissue it can find which is ready, with the process moving in many directions at once. What results is muscle that is contracting a little here, and a little there. Looking at atria that are fibrillating has been described as "a ball of worms", with little ripples of movement throughout.
This lack of mechanical efficiency is important because it may cut down substantially on how well the really important chambers, the ventricles, contract. Even more important in many cases is the fact that blood is not cleared promptly out of the atria. Where blood slows down, it can clot. In the chambers of the atria that are fibrillating, these clots not only form, but then get back into the blood stream. If they go towards the brain, they can cut off the flow of blood and cause a stroke. Clots can also go to any other organ of the body and cause a variety of problems.
What causes atrial fibrillation?
The most common cause is "idiopathic", the fancy way of saying "we don't know". Many of these cases are probably related to the "sick sinus syndrome" [link]. This is a group of disorders thought to result from wearing out or degeneration of the conduction system of the heart. Many people have no other signs of heart disease (this is sometimes termed "lone atrial fibrillation").
Other causes include:
Diseases of the mitral valve, associated with mitral regurgitation (leakage) or mitral stenosis (blockage). These conditions are often associated with large atria, and size is an important determinant of how well the atria can maintain its electrical "integrity".
Patients with weak heart muscles often have enlarged atria as a consequence of the heart's attempt to increase the amount of blood it needs to pump. As noted above, large atria find it difficult to maintain electrical integrity. Atrial fibrillation in this case, as well as in the case of mitral valve disease, can be an important cause of worsening of a patient's condition. They will be more sensitive to the loss of the atria's mechanical aid to the ventricle, which can amount to up to 25% of the mechanical work of the heart.
Other diseases of the muscles and valves of the heart may also be the underlying cause.
It is not infrequent to find patients with atrial fibrillation who also have blockage of the arteries. In many cases, this is not surprising since both occur in older people. It may then just be an association, rather than a cause (many people with gray hair have atrial fibrillation - gray hair does not cause atrial fibrillation either).
This is not an uncommon arrhythmia in patients with a variety of diseases of the lungs. This probably arises from alterations in the structure of the right side of the heart that supplies the lungs with blood, as well as perhaps low levels of oxygen in the blood.
Patients with abnormalities of the function of the thyroid gland, particularly its overproduction, also have an increased incidence of AFib.
Recently, a family was described with atrial fibrillation who shared a particular gene marker for the trait. This will eventually be useful in further understanding the arrhythmia. In general however, atrial fibrillation is not felt to be congenital at this time. While patients sometimes note that "Aunt Mildred had an arrhythmia, too", there are many arrhythmias around and hers very well may not have been atrial fibrillation. Furthermore, with so much AFib around, it is not surprising that there may be several cases in the same family every once in a while.
Infections, particularly pneumonia, may cause atrial fibrillation.
A recent study of patients with no other identifiable cause of atrial fibrillation were recently studied by undergoing biopsies of their atrium. These biopsies showed evidence of recent infection or inflammation. This may be the cause of "lone atrial fibrillation" in many cases, and could account for many of the cases currently termed "idiopathic".
Really very common, and getting more so for a couple of good reasons. First of all is the fact that we are growing older as a population, and people are living long enough for these sorts of processes involving minor degeneration of the heart's conduction system to be made apparent. Secondly, due to advances in technology and treatment, people with heart disease are living longer, and living long enough to get atrial fibrillation.
How come some people with atrial fibrillation don't even know it?
The atria don't necessarily contribute much to the efficiency of some people's hearts. People who are inactive may not notice a minor loss of efficiency. Other compensatory mechanisms can come into play, making up for the loss of the atria's contribution to cardiac output.
Some people don't have the slightest clue about even the most chaotic and rapid rhythms, while others seemingly note every skip. That's what makes the world go 'round!
Anticoagulation (blood thinning) is a key aspect of treatment as explained above. Several strategies are used, according to the specifics of a patient's situation. There is more about blood thinning below.
Apart from this, there is a need to address the electrical disturbance. Some will require no specific therapy for this. One of the most common characteristics of AFib is the fact that many of the impulses which are going randomly throughout the atrium also "hit" the AV node. Fortunately for us, the AV node does a good job of stopping the chaos, and allows far fewer impulses to get through than it is hit with. Nevertheless, many people will have rates from the lower chamber ("the ventricular rate") of 150-200 beats per minute.
One of the easiest ways to control the rate is to "get rid" of the atrial fibrillation all together by achieving normal sinus rhythm again. However, this isn't always possible, and in these cases, keeping the heart rate between 60-100 is often all that's needed to allow the patient to feel good.
In many cases, some attempt to convert the rhythm back to sinus rhythm is made. If successful in the long run, this should provide the maximum efficiency for the heart muscle, and will allow minimal use of blood thinners. Conversion can be completed with medications, electrical cardioversion, or both. There is more about electrical cardioversion and some of the medications used below.
Still, blood thinning needs to be addressed when "conversion" is contemplated. If one is certain that the atrial fibrillation has been "caught" shortly after it began (within 1-3 days), then conversion can be attempted early in the course. If it is found later in the course, or if the time that it started cannot be clearly ascertained, then some period of anticoagulation (in the range of 2-6 weeks) is often accomplished to cut down on the risk of clots traveling elsewhere when normal rhythm is restored. Some physicians may recommend the performance of a special type of echocardiogram or sonogram of the heart, a "transesophageal" echo, to further estimate the risk of a clot when conversion is being considered.
Finally, if blood thinners were used for several weeks prior to conversion, they will need to be continued for several weeks afterwards as well.
What if those things don't work?
There are several alternatives for patients who do not respond to the above measures.
1. AV Nodal ablation. Some patients have a hard time achieving satisfactory control of the ventricular response to atrial fibrillation without side effects from the necessary medications. Some are sensitive to the irregularity of their pulse. In such cases, the atrium is left in atrial fibrillation and the AV Node is "ablated" (a small amount of tissue is destroyed) using radio frequency delivered from a catheter. The rate of the resulting rhythm is almost always too slow and too unreliable - therefore an artificial pacemaker is placed to keep the ventricle beating at an adequate pace. Since the atrium is still in fibrillation, long term anticoagulation is necessary.
2. Atrial defibrillators. Atrial defibrillators are a new development for patients who maintain normal rhythm most of the time, but have occasional bouts of AFib. These devices are similar to and placed in a manner similar to that of a "standard" pacemaker -- that is, a small incision is made below the collarbone, and a "pocket" made for the generator. "Leads" are placed into the large veins which run under the collarbone, and advanced to a satisfactory position which allows them to sense and deliver electrical energy to the heart. This relatively minor surgery is often done on an outpatient basis, with the patient going home on the same day. The device senses when the atria go into fibrillation, and deliver an electrical charge to convert it back to normal. Candidates for this device must have pretty good control of their dysrhythmia -- otherwise, they would recieve multiple shocks and deplete the batteries rapidly. These are relatively new devices with great promise whose exact place in the therapy of atrial fibrillation is yet to be exactly determined. They are clearly a nice addition, but are not for everyone.
3. Surgery ("maze procedures"). Some patients really need to maintain normal rhythm for mechanical efficiency, or because they cannot take blood thinners. One procedure which has been used is a surgical procedure, again requiring a large chest incision, where multiple shallow cuts are made in the atrium to divide it into multiple electrical areas. This cuts down on the ability of the atrium to maintain fibrillation. This is relatively new, requires an open chest procedure, and is not always successful. Similar procedures developed for atrial flutter were later "translated" into procedures which only required catheters to accomplish, but the prospects for this becoming common for AFib are less promising.
What about cardioversion? That sounds scary!
It does sound scary, and I sure wouldn't want to be the first patient to have tried it! However, it is now a very well established procedure, and one that has been around for a long time and is considered quite safe. Cardioversion and defibrillation often must be done on an emergency basis in other rhythms, but for atrial fibrillation, this is done on an elective basis. Sedation or brief general anesthesia is administered before the electricity is delivered. Paddles are placed on the chest, and a modest dose of electricity is given in step with the patient's underlying heart beat.
The goal of this therapy is to deliver enough electrical energy to briefly depolarize all or almost all of the atrial tissue. The first cell to restart the process of depolarization should be in the sinus node, the place where the rhythm usually begins. In theory, the heart will then maintain the normal mechanism thereafter.
Although this clearly does not sound like fun, it is very well tolerated when the patient receives adequate sedation or anesthesia. It is most frequently done as an outpatient, and the patient can be sent home on the same day. It is possible that a worse arrhythmia can result from this procedure requiring further therapy. It is theoretically possible that death could result from the procedure or the anesthesia, although this would be extremely rare. The benefits of this procedure usually vastly outweigh its risks.
Not everyone is a suitable candidate for cardioversion. Many times it is because that AFib has been present for so long that the atria will not be able to maintain the normal rhythm again. Patients are selected for their need to attain sinus rhythm, and the likelihood that cardioversion will work long-term. In properly selected cases, an 80% success rate should be possible.
Anticoagulation may be necessary before and after the procedure depending on the duration of time AFib was present prior to the procedure.
What are some of the medications used to treat AFib?
Medications are used for three primary reasons in atrial fibrillation:
1. Slow the rate that the ventricles contract if they are going too fast (the goal is generally to keep the rate less than 100 beats/minute).
2. Convert the rhythm to normal, or keep it there.
3. Thin the blood with anticoagulants to decrease the chance of clots.
Each of these types of medication will be discussed below.
Medications to control the rate of atrial fibrillation
Medications such as beta-blockers or calcium-channel blockers and digoxin are used to slow down the heart rate of ventricular activation by the atria. These agents are not designed to "convert" the rhythm to normal. They work primarily to "block" the AV Node, and allow fewer of the impulses from the atrium to get through to the ventricles.
Beta-Blockers
Calcium-channel blockers
Digitalis
Medications to convert the rhythm to normal
Other anti-arrhythmics are given, not to try to control the heart rate, but to try to convert or maintain the rhythm to the normal mechanism. These agents used to be given pretty frequently, but are now used with caution. Anti-arrhythmics have a property called "proarrhythmic", which is a quality that refers to their tendency to make some rhythms worse in some patients. In some cases, this can take a relatively benign arrhythmia such as AFib, and cause a new arrhythmia that can be life threatening. For this reason, they are used with great care if at all.
Quinidine, procainamide, and disopyramide
Soltalol
Propafenone
Amiodarone
What sorts of blood thinners are you talking about?
As good as aspirin may be for preventing clots in the arteries to the heart, and therefore heart attacks, it just hasn't been found to be as effective in preventing clots in atrial fib. That's not to say it doesn't do anything, and it may be just the right drug for some groups of patients. However, most patients will require warfarin, or "Coumadin" to achieve the highest reduction in risk of stroke.
This medication has also been around for a long time. It is actually the same active agent found in the most popular rat and mice poisons. When administered carefully with appropriate follow-up of blood tests measuring its effectiveness (the "protime"), it can lead to a substantial decrease in the incidence of strokes in selected patients.
Most people are reluctant at first to start this medication, but once they understand the good it can do, will take it to prevent strokes and other complications.
How long do I have to take a blood thinner?
This will vary a great deal depending on the circumstances. Some will require warfarin only for a short time around the time of a successful cardioversion. Others will have it continued for several months to make sure no clots form if the atrial fibrillation comes back. Many people with require it for the rest of their lives.
Why can't I just take an aspirin?
Some people can. However, in this particular case, many if not most patients will do better with warfarin.
Why won't they just put in a pacemaker. That will fix it, won't it?
Well, not usually. See, a pacemaker is placed simply to keep the heart from going too slow. It does not correct the irregularity of the rhythm of AFib, nor keep it from going too fast.
"Atrial defibrillators" are sometimes used, and are explained above. These are not classic pacemakers, and are useful only in a few cases.
It appears that once many patients are corrected back into normal sinus rhythm that the placement of a permanent pacemaker utilizing leads in both the atrium and the ventricle may cut down on recurrent episodes of AFib. This is not true, nor advisable, for all patients. It appears to work by cutting down on excessively long pauses between beats which may be an important factor in starting the rhythm in some patients.
In conclusion . . .
Pretty complicated? Don't be frustrated. I started out this section noting that atrial fibrillation got more attention than it deserved in some ways. This remains true, and it's largely because it's not altogether simple. Much of the confusion, though stems simply from the numerous options available. In many ways, all of these options are good . . . the right one for you is out there. Stick with it!
Also see these related topics:
Arrhythmias - Introduction Arrhythmias - General Considerations Arrhythmias - Specific Pacemakers Ventricular arrhythmias
©COPY;1997 HeartPoint Updated December 1997
| Commentary |
Food You Will Love | HeartPoint
Gallery | In The News | Health Tips | What's New
|
| Information Center | Home
|
This site presents material for your information, education and entertainment. We can assume no liability for inaccuracies, errors, or omissions. Above all, material on this site should not take the place of the care you receive from a personal physician. It is simply designed to help in the understanding of the heart and heart disease, and not as a diagnostic or therapeutic aid. You should seek prompt medical care for any specific health issues. Please feel free to browse the site and download material for personal and non-commercial use. You may not however distribute, modify, transmit or reuse any of these materials for public or commercial use. You should assume that all contents of the site are copyrighted. ©COPY;1997 HeartPoint